Augmented and Virtual Reality enhance the healthcare experience
Author’s note: This article is part of a series published in SeAMK eJournal about cutting-edge technologies (Artificial Intelligence, Big Data, Robotics, Internet of Things, and Virtual and Augmented Reality) that will revolutionize the healthcare in the near future.
The plethora of new hardware and software technologies are set to become pillar over the coming years to ease the conception of the hospital of the future that will see the seamless integration of digital health information into routine clinical practice. With improvements in computational power and advances in visual and haptic display technologies, Augmented Reality (AR) and Virtual Reality (VR) can offer potential benefits for tests in a safe and simulated settings, as well as improve management of real-life procedures. Nevertheless, AR and VR although having recently seen rapid improvements in affordability, immersive features and hardware and portable capabilities, have yet to be introduced widely into healthcare [1].
AR, often called Mixed Reality (MR), employs a transparent display that allows for the integration and overlay of digital content over the real physical word being visible together. Thus, AR provide user-environmental interfaces, quite useful in a healthcare context, by using personal head mounted displays (as Microsoft HoloLens or Magic Leap One), digital spectacles aka smart glasses, smart watches, or handheld devices like camera-enabled smartphones or tablets. On the contrary, with VR, lastly improved by its shocking hyper-realism, the real world is completely occluded by the head-mounted display or a cave automatic virtual environments providing a fully immersive experience that replaces the real environment with a 3D virtual environment allowing enhanced interaction and possible haptic feedback.
Employment of VR and AR are numerous in the healthcare field, namely: medical education and training in different specialties (Anatomy, Anesthesia, Cardiology, Dermatology, Family Medicine, Forensic medicine, gastroenterology, neurology, ophthalmology, orthopedics, pediatrics and radiology) [2]; surgical simulation, navigation and training [1] [3]; nursing care assistance and education(wound care, intravenous injection, vital signs monitoring) [4]; cognitive support for early dementia patient in outside hospital environment [5]; rehabilitation psychotherapy and psychological treatment of anxiety, phobias and eat disorders [5] [6]; pain management [7]; telemedicine [8]; non-technical skills development (teamwork, communication and situation awareness) [9]; and patient education [1]. Most AR and VR application stem from surgery, where all studies shown several educational benefits significantly outperforming traditional learning approaches [2], especially reinforcing the dexterity of the operator and fostering the patient safety in complex surgical techniques. Moreover, by integrating patient-specific data and clearer 3D organs or tumor models built from observation of CT, MRI or ultrasound scan (as shown in figure 1), AR and VR can allow for contextual and detailed preplanning of medical procedures, better identification of incidentals, and collaborative postoperative review even remotely. Another important application is real-time remote consultation, especially useful in an emergency scene [8], where AR and VR have demonstrated utility and feasibility by enabling the expert physician to interact with a 3D representation of the patient and their medical information in novel ways, and improve communication through enhanced visual caregiver instructions [1]. AR, in particular, reduces attention deviation and time to initiation of critical life-saving maneuvers where real-time decision is vital like assisted pediatric cardiopulmonary resuscitation or prehospital situation where emergency department are expecting the arrival of the critical patients [10]. Other studies show VR as an effective treatment for reducing acute pain both in adults and children after and during medical procedures or burn cures [7] [6], as well as an assistive rehabilitation technology for individuals with certain conditions as stroke, cerebral palsy, Parkinson’s disease and multiple sclerosis among others [11]. An example of the latter application is the RehabWall [12] (Figure 2) which has been purchased by SeAMK and is shown in its Healthcare and Social Work school.
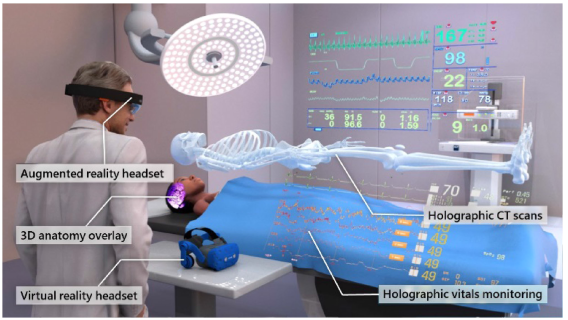

AR and VR are transforming the practice of healthcare by providing powerful and intuitive methods of exploring and interacting with digital medical data, as well as integrating data into the physical world to create natural and interactive virtual experiences that traduces in enhancement of quality of care. Interaction between real and 3D virtual worlds may convey greater feelings of presence, time savings, real-time performance feedback, facilitate the clinical communication process, increased accuracy of documentation, hands-free usage of a device, and foster higher levels of interpersonal trust between therapists and patients. These technologies significantly improve the learning process, through contextual information provision, along with other factors related to visualization, directing attention, intrinsic benefits of motivation, self-confidence and efficacy, physical interaction activating kinesthetic schemes, patient safety, and skill retention. AR and VR also support patients by enabling them in decision-making process, and improving the information received as well as the engagement in the preoperative process and anxiety reduction. Moreover, digitalization allows to personalize the AR and VR environment increasing the opportunity, along with appropriate haptic devices that augment the effect on immersion, for enhancing the adherence and effectiveness in the treatment.
On the other hand, to promote the adoption of AR and VR in the healthcare domain special attention should be paid on technological limitations related to limited computing power, occlusion of the user’s field of view and poor ergonomics of haptics and head-mounted displays. Also, the amount of information presented in AR or an excessive complicated user interface could distract the user on the task performed (e.g. surgery) or increase their anxiety and fear (e.g. older adults with dementia). Finally, future AR and VR devices will likely also have to be able to connect and interface with other medical devices in order to be successful, thus efforts in ensure this interoperability must be tackled.
Pedro A. Moreno Sánchez
RDI Expert/ Researcher
PhD, PMP®
Seinäjoki University of Applied Sciences
School of Health Care and Social Work
References
[1] M. R. Desselle, R. A. Brown, A. R. James, M. J. Midwinter, S. K. Powell, and M. A. Woodruff, “Augmented and Virtual Reality in Surgery,” Comput. Sci. Eng., vol. 22, no. 3, pp. 18–26, May 2020, doi: 10.1109/MCSE.2020.2972822.
[2] J. Gerup, C. B. Soerensen, and P. Dieckmann, “Augmented reality and mixed reality for healthcare education beyond surgery: an integrative review,” Int J Med Educ, vol. 11, pp. 1–18, Jan. 2020, doi: 10.5116/ijme.5e01.eb1a.
[3] C. Lee and G. K. C. Wong, “Virtual reality and augmented reality in the management of intracranial tumors: A review,” J. Clin. Neurosci., vol. 62, pp. 14–20, Apr. 2019, doi: 10.1016/j.jocn.2018.12.036.
[4] H. Wüller, J. Behrens, M. Garthaus, S. Marquard, and H. Remmers, “A scoping review of augmented reality in nursing,” BMC Nurs., vol. 18, no. 1, p. 19, May 2019, doi: 10.1186/s12912-019-0342-2.
[5] V. Rose, I. Stewart, K. Jenkins, C. S. Ang, and M. Matsangidou, “A Scoping Review Exploring the Feasibility of Virtual Reality Technology Use with Individuals Living with Dementia,” in A Scoping Review Exploring the Feasibility of Virtual Reality Technology Use with Individuals Living with Dementia, Cyprus, Dec. 2018, Accessed: Apr. 29, 2020. [Online]. Available: https://doi.org/10.2312/egve.20181325.
[6] J. Dascal et al., “Virtual Reality and Medical Inpatients: A Systematic Review of Randomized, Controlled Trials,” Innov. Clin. Neurosci., vol. 14, no. 1–2, pp. 14–21, Feb. 2017.
[7] B. Mallari, E. K. Spaeth, H. Goh, and B. S. Boyd, “Virtual reality as an analgesic for acute and chronic pain in adults: a systematic review and meta-analysis,” J. Pain Res., vol. 12, pp. 2053–2085, Jul. 2019, doi: 10.2147/JPR.S200498.
[8] B. W. Munzer, M. M. Khan, B. Shipman, and P. Mahajan, “Augmented Reality in Emergency Medicine: A Scoping Review,” J. Med. Internet Res., vol. 21, no. 4, p. e12368, 2019, doi: 10.2196/12368.
[9] M.-S. Bracq, E. Michinov, and P. Jannin, “Virtual Reality Simulation in Nontechnical Skills Training for Healthcare Professionals: A Systematic Review,” Simul. Healthc., vol. 14, no. 3, pp. 188–194, Jun. 2019, doi: 10.1097/SIH.0000000000000347.
[10] B. John and N. Wickramasinghe, “A Review of Mixed Reality in Health Care,” in Delivering Superior Health and Wellness Management with IoT and Analytics, N. Wickramasinghe and F. Bodendorf, Eds. Cham: Springer International Publishing, 2020, pp. 375–382.
[11] T. Rose, C. S. Nam, and K. B. Chen, “Immersion of virtual reality for rehabilitation – Review,” Appl. Ergon., vol. 69, pp. 153–161, May 2018, doi: 10.1016/j.apergo.2018.01.009.
[12] “CSE Entertainment.” https://cse.fitness/en/rehabwall/ (accessed May 13, 2020).